Facial paralysis can be a distressing condition that affects individuals of all ages. Among the various causes of facial paralysis, Ramsay Hunt Syndrome vs Bell’s Palsy is two conditions that often lead to similar symptoms but have distinct underlying causes and treatment approaches. Understanding the differences between Ramsay Hunt Syndrome vs Bell’s Palsy is crucial for accurate diagnosis and appropriate management.
In this article, we will explore the disparities between these two conditions and shed light on their unique characteristics. Ramsay Hunt Syndrome is caused by the varicella-zoster virus (VZV) and is often associated with additional symptoms such as ear pain and rash, while Bell’s Palsy is an idiopathic condition affecting the facial nerve.
By comparing and contrasting these conditions, we aim to enhance awareness and provide valuable insights into the diagnosis, treatment, and prognosis of Ramsay Hunt Syndrome and Bell’s Palsy.
Ramsay Hunt Syndrome
Ramsay Hunt Syndrome is a neurological condition characterized by facial paralysis that occurs due to infection by the varicella-zoster virus (VZV). This virus is the same virus responsible for causing chickenpox and shingles.
Causes of Ramsay Hunt Syndrome
Ramsay Hunt Syndrome is caused by the reactivation of the varicella-zoster virus, which may remain dormant in the sensory nerve ganglia after the initial infection of chickenpox.
When the virus reactivates, it affects the facial nerve, resulting in the symptoms of facial paralysis.
Symptoms and Clinical Presentation
The primary symptom of Ramsay Hunt Syndrome is facial paralysis, which typically affects one side of the face.
The paralysis may be accompanied by other symptoms such as severe ear pain, rash, and blistering in the ear canal or on the face. These blisters are referred to as herpes zoster oticus or auricular herpes zoster.
Read More: Apraxia of Speech and Dyslexia: Understanding the Connection
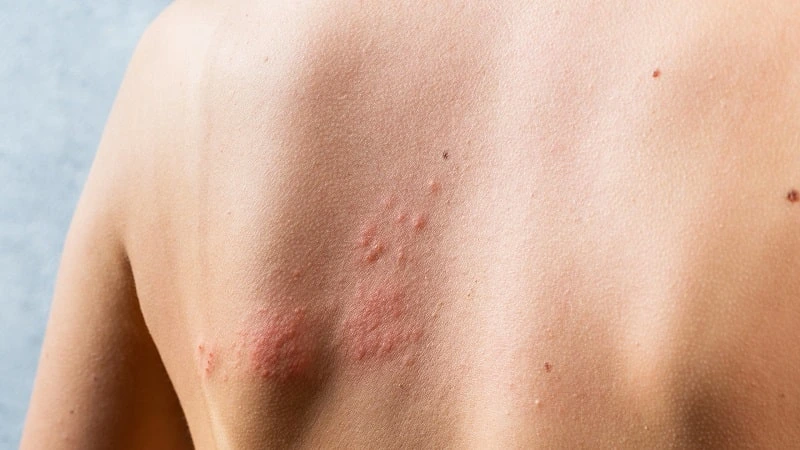
Role of the Varicella-Zoster Virus (VZV)
The varicella-zoster virus plays a crucial role in the development of Ramsay Hunt Syndrome. The virus spreads along the sensory nerves, affecting the facial nerve and causing inflammation and damage, leading to facial paralysis.
Potential Complications and Long-term Effects
If left untreated or inadequately managed, Ramsay Hunt Syndrome can lead to various complications and long-term effects.
These may include persistent facial weakness, muscle contractures, hearing loss, vertigo, and difficulties with eye closure, resulting in eye dryness and potential corneal damage.
Diagnosis and Treatment Options
Diagnosing Ramsay Hunt Syndrome involves a thorough examination of the patient’s symptoms, medical history, and physical examination. In some cases, additional tests such as a viral culture or polymerase chain reaction (PCR) test may be performed to confirm the presence of the varicella-zoster virus.
Treatment typically involves antiviral medications, such as acyclovir, to reduce viral replication and inflammation. Corticosteroids may also be prescribed to decrease swelling and promote nerve recovery.

Prognosis and Recovery
The prognosis for Ramsay Hunt Syndrome varies depending on factors such as the severity of symptoms, the extent of nerve damage, and the promptness of treatment.
Early diagnosis and appropriate management can improve the chances of a favorable outcome. While some individuals may experience a complete recovery, others may have residual facial weakness or other long-term effects.
Rehabilitation exercises and therapies can aid in the recovery process and improve facial muscle function.
Read More: Symptoms of Nerve Damage After Varicose Vein Surgery
Bell’s Palsy
Bell’s Palsy is a condition characterized by sudden, temporary weakness or paralysis of the facial muscles, usually affecting one side of the face. It is the most common form of facial paralysis, accounting for the majority of cases.
Definition and Prevalence
Bell’s Palsy is defined as an idiopathic condition, meaning its exact cause is unknown. It occurs when the facial nerve (cranial nerve VII), responsible for controlling the muscles of facial expression, becomes inflamed or compressed. Bell’s Palsy affects approximately 20 to 30 individuals per 100,000 people annually.
Symptoms and Clinical Presentation
The primary symptom of Bell’s Palsy is the sudden onset of facial weakness or paralysis, typically on one side of the face.
This can make it difficult to close the eye or control facial expressions. Other common symptoms include drooping of the mouth, drooling, changes in taste perception, increased sensitivity to sound in one ear, and pain around the jaw or behind the ear.
Role of the Facial Nerve (Cranial Nerve VII)
The facial nerve, or cranial nerve VII, plays a vital role in controlling the muscles of facial expression. It also carries taste sensations from the anterior two-thirds of the tongue.
In Bell’s Palsy, inflammation or compression of this nerve disrupts its ability to transmit signals, leading to facial weakness or paralysis.
Potential Complications and Long-term Effects
While most individuals with Bell’s Palsy recover fully within three to six months, there can be potential complications and long-term effects.
These may include incomplete recovery of facial muscle function, persistent facial weakness, synkinesis (involuntary movements during voluntary facial movements), and emotional or psychological effects due to the impact on facial appearance.
Diagnosis and Treatment Options
Diagnosing Bell’s Palsy is primarily based on clinical examination and the exclusion of other potential causes of facial paralysis.
Medical history, physical examination, and sometimes additional tests such as electromyography (EMG) or imaging studies may be used to rule out other conditions.
Treatment for Bell’s Palsy often involves a combination of medications, such as corticosteroids to reduce inflammation, and supportive measures such as eye protection to prevent corneal damage due to reduced blinking.
Prognosis and Recovery
The prognosis for Bell’s Palsy is generally good, with the majority of individuals experiencing spontaneous recovery.
Most patients notice improvement within a few weeks, with significant recovery occurring within three to six months.
However, the extent and speed of recovery can vary from person to person. Rehabilitation exercises, physical therapy, and facial massage techniques may be recommended to help improve facial muscle strength and coordination.
Key Differences between Ramsay Hunt Syndrome and Bell’s Palsy
When it comes to facial paralysis conditions, Ramsay Hunt Syndrome and Bell’s Palsy share some similarities, but they also have significant differences in terms of their underlying causes, symptoms, and treatment approaches.
Etiology: Viral Infection vs. Idiopathic Condition
One of the primary differences between Ramsay Hunt Syndrome and Bell’s Palsy lies in their etiology.
Ramsay Hunt Syndrome is caused by the varicella-zoster virus (VZV), which is the same virus responsible for chickenpox and shingles.
On the other hand, Bell’s Palsy is classified as an idiopathic condition, meaning its exact cause is unknown.
While both conditions involve facial paralysis, the presence of VZV in Ramsay Hunt Syndrome distinguishes it from the idiopathic nature of Bell’s Palsy.
Additional Symptoms and Associated Conditions
Ramsay Hunt Syndrome often presents additional symptoms beyond facial paralysis. These may include severe ear pain (otalgia), rash, and blistering in the ear canal or on the face.
The presence of these symptoms is not typically seen in Bell’s Palsy. In Ramsay Hunt Syndrome, the combination of facial paralysis, ear pain, and rash can serve as important diagnostic clues to distinguish it from Bell’s Palsy.
Prognosis and Recovery Rates
The prognosis and recovery rates can also differ between Ramsay Hunt Syndrome and Bell’s Palsy. Ramsay Hunt Syndrome tends to have a more guarded prognosis compared to Bell’s Palsy.
This is partly due to the potential complications associated with Ramsay Hunt Syndrome, such as persistent facial weakness, muscle contractures, hearing loss, and vertigo.
In Bell’s Palsy, the majority of individuals experience spontaneous recovery within a few weeks to several months, with a more favorable prognosis overall.
Treatment Approaches and Management Strategies
The treatment approaches for Ramsay Hunt Syndrome and Bell’s Palsy may vary. In Ramsay Hunt Syndrome, antiviral medications, such as acyclovir, are commonly prescribed to reduce viral replication and inflammation caused by the varicella-zoster virus.
Corticosteroids may also be utilized to reduce swelling and promote nerve recovery. For Bell’s Palsy, corticosteroids are often the primary treatment, as they help decrease inflammation and improve outcomes.
Supportive measures, such as eye protection and rehabilitation exercises, may be employed in both conditions to aid in recovery and prevent complications.
Potential Complications and Sequelae
While both conditions can have complications, the nature of these complications differs between Ramsay Hunt Syndrome and Bell’s Palsy. Ramsay Hunt Syndrome carries a higher risk of long-term effects, including persistent facial weakness, hearing loss, and vertigo.

Additionally, the involvement of the varicella-zoster virus in Ramsay Hunt Syndrome can result in other neurological complications associated with the virus, such as encephalitis or meningitis.
Bell’s Palsy, while generally having a more favorable prognosis, can still lead to residual facial weakness, synkinesis (involuntary facial movements), and emotional or psychological effects related to facial appearance.
Read More: Immediate Relief for Sciatica Pain
Similarities between Ramsay Hunt Syndrome and Bell’s Palsy
While Ramsay Hunt Syndrome and Bell’s Palsy have distinct differences, they also share several similarities in terms of their presentation, diagnostic challenges, and the importance of early intervention and treatment.
Facial Paralysis as the Primary Symptom
The most notable similarity between Ramsay Hunt Syndrome and Bell’s Palsy is the presence of facial paralysis as the primary symptom.
Both conditions result in weakness or paralysis of the facial muscles, making it difficult to control facial movements and expressions.
The degree of facial paralysis can vary, ranging from mild weakness to complete paralysis on one side of the face.
Diagnosis Challenges and Differential Diagnosis Considerations
Both Ramsay Hunt Syndrome and Bell’s Palsy can present diagnostic challenges due to their overlapping symptoms and clinical manifestations.
The shared symptom of facial paralysis, along with potential variations in the presentation of associated symptoms, can make it challenging to differentiate between the two conditions.
Healthcare professionals need to carefully evaluate the patient’s medical history, perform a thorough physical examination, and consider additional diagnostic tests to arrive at an accurate diagnosis and differentiate between Ramsay Hunt Syndrome and Bell’s Palsy.
Importance of Early Intervention and Treatment
In both Ramsay Hunt Syndrome and Bell’s Palsy, early intervention, and treatment are crucial for optimal outcomes.
Prompt diagnosis and initiation of appropriate management strategies can help minimize complications, promote recovery, and improve the chances of restoring normal facial muscle function.
early treatment may include antiviral medications, corticosteroids, and supportive measures such as eye protection and rehabilitation exercises.
Timely medical intervention plays a vital role in preventing long-term effects and enhancing the overall prognosis.
Conclusion
In conclusion, Ramsay Hunt Syndrome and Bell’s Palsy are two distinct conditions that can cause facial paralysis. Ramsay Hunt Syndrome is caused by the varicella-zoster virus (VZV), while Bell’s Palsy is an idiopathic condition.
They differ in terms of associated symptoms, prognosis, and treatment approaches. However, both conditions share similarities, such as facial paralysis as the primary symptom, diagnostic challenges, and the importance of early intervention and treatment for optimal outcomes.
Recognizing the differences between Ramsay Hunt Syndrome and Bell’s Palsy is crucial for accurate diagnosis and appropriate management.
Healthcare professionals should carefully evaluate the patient’s symptoms, and medical history, and perform a comprehensive examination to arrive at an accurate diagnosis.
Early initiation of treatment, including antiviral medications and corticosteroids, along with supportive measures, can enhance the chances of recovery and minimize complications.
By raising awareness and understanding the distinctions between these conditions, healthcare professionals can provide timely and effective care to individuals experiencing facial paralysis, ultimately improving their quality of life and facial function.
Frequently Asked Questions (FAQs)
1. Can Ramsay Hunt Syndrome and Bell’s Palsy occur on both sides of the face simultaneously?
No, both Ramsay Hunt Syndrome and Bell’s Palsy typically affect only one side of the face.
2. Are there any specific risk factors for developing Ramsay Hunt Syndrome or Bell’s Palsy?
While the exact causes of Bell’s Palsy and Ramsay Hunt Syndrome are not fully understood, some potential risk factors for Bell’s Palsy include viral infections, pregnancy, diabetes, and a family history of the condition. Ramsay Hunt Syndrome is specifically caused by varicella-zoster virus (VZV) reactivation.
3. Can Ramsay Hunt Syndrome or Bell’s Palsy recur?
Ramsay Hunt Syndrome and Bell’s Palsy can recur, although it is relatively rare. Recurrence is more commonly associated with Bell’s Palsy.
4. Is there any specific age group that is more susceptible to Ramsay Hunt Syndrome or Bell’s Palsy?
Both Ramsay Hunt Syndrome and Bell’s Palsy can occur in individuals of any age, but they are more commonly observed in adults.
5. Can Ramsay Hunt Syndrome or Bell’s Palsy be prevented?
There are no specific preventive measures for Ramsay Hunt Syndrome or Bell’s Palsy. However, maintaining good overall health, managing stress levels, and practicing good hygiene can contribute to overall well-being.
6. Are there any long-term effects of Ramsay Hunt Syndrome or Bell’s Palsy?
Ramsay Hunt Syndrome can lead to potential long-term effects, including persistent facial weakness, hearing loss, and vertigo. Bell’s Palsy can also result in residual facial weakness, synkinesis (involuntary facial movements), and emotional or psychological effects due to facial appearance changes.
7. How long does it take to recover from Ramsay Hunt Syndrome or Bell’s Palsy?
Recovery time can vary for each individual and depends on factors such as the severity of symptoms, promptness of treatment, and the extent of nerve damage. While some people may experience significant improvement within a few weeks, complete recovery may take several months.
8. Can facial exercises or physical therapy help in the recovery from Ramsay Hunt Syndrome or Bell’s Palsy?
Yes, facial exercises and physical therapy, such as gentle massages and range-of-motion exercises, can aid in the recovery process for both Ramsay Hunt Syndrome and Bell’s Palsy. These interventions can help improve muscle strength and coordination.
9. Can Ramsay Hunt Syndrome or Bell’s Palsy affect other cranial nerves?
While Ramsay Hunt Syndrome primarily affects the facial nerve (cranial nerve VII), it can sometimes involve other cranial nerves, leading to additional symptoms such as hearing loss or vertigo. Bell’s Palsy typically only affects the facial nerve.
Medical References
- National Institute of Neurological Disorders and Stroke. (2019). Bell’s Palsy Fact Sheet. Retrieved from https://www.ninds.nih.gov/Disorders/Patient-Caregiver-Education/Fact-Sheets/Bells-Palsy-Fact-Sheet
- Gilden, D. H. (2015). Clinical practice. Bell’s Palsy. New England Journal of Medicine, 372(17), 1654–1661.
- Peitersen, E. (2002). Bell’s palsy: the spontaneous course of 2,500 peripheral facial nerve palsies of different etiologies. Acta Oto-Laryngologica, 122(7), 4–30.
- Kang, B. H., Hong, Y. H., Kim, J. M., et al. (2013). Ramsay Hunt syndrome with severe dysphagia caused by simultaneous cranial polyneuritis involving cranial nerves V, IX, X, and XI. Annals of Rehabilitation Medicine, 37(6), 881–884.
- Cohen, J. I. (2013). Clinical practice: Herpes zoster. The New England Journal of Medicine, 369(3), 255–263.
- Kuijf, M. L., Kluijt, I., Mulder, F. J., et al. (2020). Bell’s Palsy: A Mini-Review on Treatment Options in Acute Facial Paralysis. Current Neurology and Neuroscience Reports, 20(7), 1–9.